Key Takeaways
- Lyme disease is a serious (and sometimes fatal) infection caused by the bite of a tick that can affect both people and pets.
- Dogs and outdoor cats are at risk of developing Lyme disease when they spend time outdoors in affected areas.
- Antibiotics are used to kill the bacteria that cause Lyme disease and some pets have to spend a few days in the hospital.
While you and your pooch explore the outdoors, keep in mind the possibility of Lyme disease, a serious (and sometimes fatal) infection caused by the bite of a tick. Pet parents can also develop Lyme disease if they are bitten – consider these tips for both yourself and your dog.
What is Lyme disease?
Lyme disease is an infection caused by a tick bite. Only two common tick species carry the disease-causing bacteria in the United States, both come from the “Ixodes” family of ticks. Depending on where you live in the country, anywhere from 10-50% of the Ixodes ticks actually carry the Lyme disease bacteria Burrelia bergdorferi (bur-rel-ee-ah burg-dor-fur-ee), which is passed along in their saliva into their host’s bloodstream.
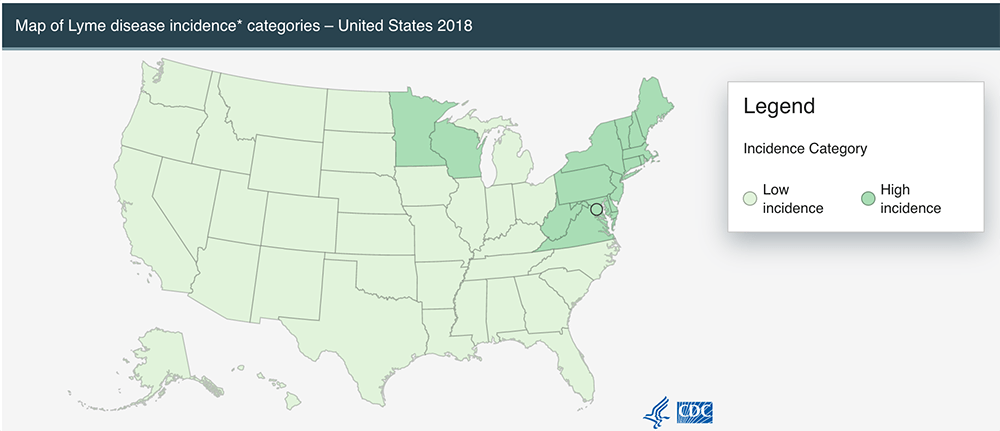
- The Blacklegged tick is widespread throughout the East and Southeast U.S., as well as near the Great Lakes.
- On the West Coast, the Western Blackegged tick can be a carrier of the bacteria.
- As of January 2019, DVM360 reports that Lyme disease is spreading to regions once thought low-risk, stating: “The Companion Animal Parasite Council (CAPC) recently released a study that shows that Lyme disease is spreading to regions not previously thought to be at risk for tick-borne disease. States such as Illinois, Iowa, North Dakota, Ohio, Michigan, West Virginia and Tennessee have all seen an increase in the prevalence of Lyme disease.”
Dogs and outdoor cats are at risk of developing Lyme disease when they spend time outdoors in affected areas. Ticks typically catch a ride on pets’ fur after they pass through grassy, wooded or sandy areas.
Pet parents can also be infected with Lyme disease, but only through a tick bite – you cannot catch Lyme disease directly from your pet!
What are the symptoms of Lyme disease?
“Paisley is an almost three-year-old Rottweiler who loves playing with her big sister Nala; she loves going for a swim or chasing balls which and carrying two in her mouth at the same time. She’s very proud of this talent! She was usually seen cruising the streets on her daily walk,” says pet parent Sean. He also remembers when Paisley fell very sick: “Her symptoms came on abruptly. In the morning she was running around and acting completely normal and by the evening she was very lethargic and didn’t want to get up,” he explains. “She had an upset stomach but the most unsettling symptom was her joint paint that got so bad her legs wouldn’t work and she couldn’t stand.”

In humans, the infection initially presents as a bullseye-like rash, appearing within three to thirty days after a bite. However, the symptoms of Lyme disease in dogs differ:
- Generalized pain
- “Walking on eggshells,” or lameness (abnormal walking)
- Loss of appetite
- Joint swelling
- Fever
- Enlarged lymph nodes
Symptoms of Lyme disease may appear and disappear suddenly or can reoccur over a period of time. Difficulty walking has been described as “walking on eggshells,” and may affect one or a couple of limbs, and the limbs affected may switch to other limbs. “We had noticed that about a week prior she started to chew on her paws around the joints that were most affected,” continues Sean. “She is outside daily and is on a flea and tick prevention so it was unexpected that she contracted Lyme. In the past year, we had only found one tick on her and that was months prior.” After Paisley had been laying in the same spot for a few hours, Sean went to get her up to eat, “and that is when we noticed her limbs not working. We immediately called our vet and went to an emergency vet where she was held for three days.”
How is Lyme disease diagnosed?
A veterinary exam is the best way to get the ball rolling. If you suspect your pet has Lyme disease, don’t wait! Symptoms can persist off and on for over a year; some pets aren’t diagnosed until several months to a year after exposure.
Your veterinarian will perform two blood tests to diagnose Lyme disease. An antibody test is done to determine the presence of antibodies (defense proteins) in the bloodstream, which indicates an infection. If the dog has not been vaccinated for Lyme disease, then the first time they can test positive on this antibody test is about 2-3 weeks after the tick bite. If a dog has been vaccinated for Lyme disease, the soonest they can test positive for Lyme-specific antibodies would be 6-8 weeks after the bite.
Testing positive, however, does not mean that your pet will ever get sick from the infection. Another test – a polymerase chain reaction (PCR) test can attempt to isolate bacterial DNA from a skin sample near the location of the tick bite or the skin near the first joint affected. Other body tissues and fluids can be used as well for this test, but tend to be much less helpful.
How is Lyme disease treated?
Antibiotics are used to kill the bacteria that causes Lyme disease. The course of treatment is very long, as all bacteria in the body must be eradicated to cure the infection. Your vet may need to change the prescribed antibiotic, as some bacteria are immune to certain medications. Many pups are in the hospital for a few days on IV fluids and antibiotics.

“Paisley is a few weeks out of her hospital visit and doing much better,” says Sean. “She is not back to her normal self and is still on heavy medication. She has started back up her walks and slowly getting her energy back.”
How can I prevent Lyme disease?
When you go hiking with your dog, avoid thickly wooded, areas of tall grass or bushy areas. Stick to marked trails, especially in parts of the country where ticks are endemic.
After an outdoor excursion, thoroughly check your pet for any ticks! Wear a pair of thick gloves, long sleeves and long pants to avoid being bit yourself. Ticks can be as small as a pinhead when they are young, so use a flashlight for best results. If you find a tick, remove it immediately using a pair of tweezers. Avoid crushing the tick or partially removing it – bacteria can enter the skin through any open wound or cut.
Over-the-counter tick control medications and collars are widely available, and a vaccine for Lyme disease is also available. If you live in an area where ticks are endemic and spend tons of time outdoors, consider vaccinating your pet. Talk to your veterinarian about prescription tick preventives and the Lyme disease vaccine to see which is best for your dog.
How much does Lyme disease cost to treat?
The price of antibiotics for pets and humans has been increasing in recent years – a two-week dose of doxycycline can cost $400 in some areas. Ask your veterinarian if they use a compounding pharmacy, which can help manage cost.
The Healthy Paws plan covers Lyme disease treatment as long as it is not a pre-existing condition and the 15-day waiting period has passed before it is contracted. The insurance does not cover vaccines or preventive treatment.
Blood tests usually run around $80, depending on the methods used. Pet parents also must pay the veterinary exam fee, which is $40 to $100+, depending on your location. However, a pup diagnosed with Lyme is looking at hospitalization and chronic condition treatment. For example, Sean’s claims for Paisley included emergency treatment, hospitalization, and ongoing medications totaling $6,969, of which he’s been reimbursed $6,004 (90% reimbursement rate; $250 deductible).
The content is not intended to be a substitute for professional veterinarian advice, diagnosis, or treatment. Always seek the advice of your veterinarian or other qualified health provider with any questions you may have regarding a medical diagnosis, condition, or treatment options.









